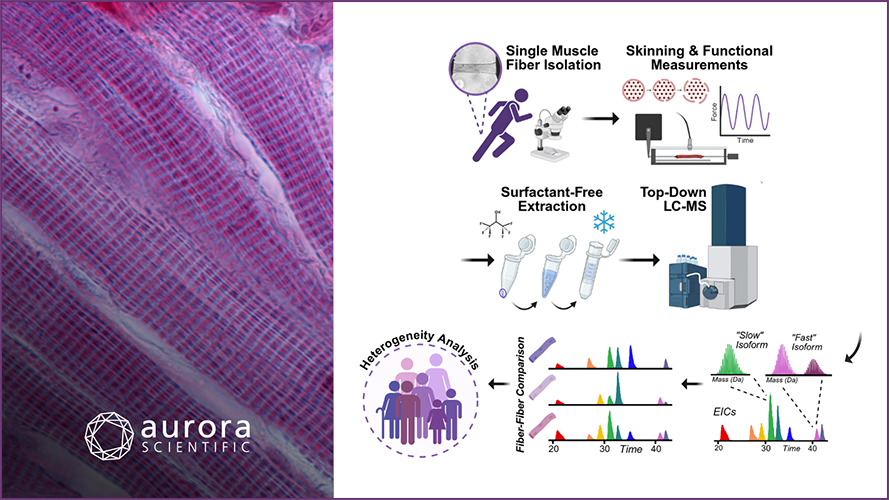
Springing Forward: Myofilament Advances
From unraveling the roles of titin’s P-zone domains in thick filament arrangement to examining the impact of cMyBP-C mutations on cardiac muscle relaxation, these papers illuminate ongoing efforts ...
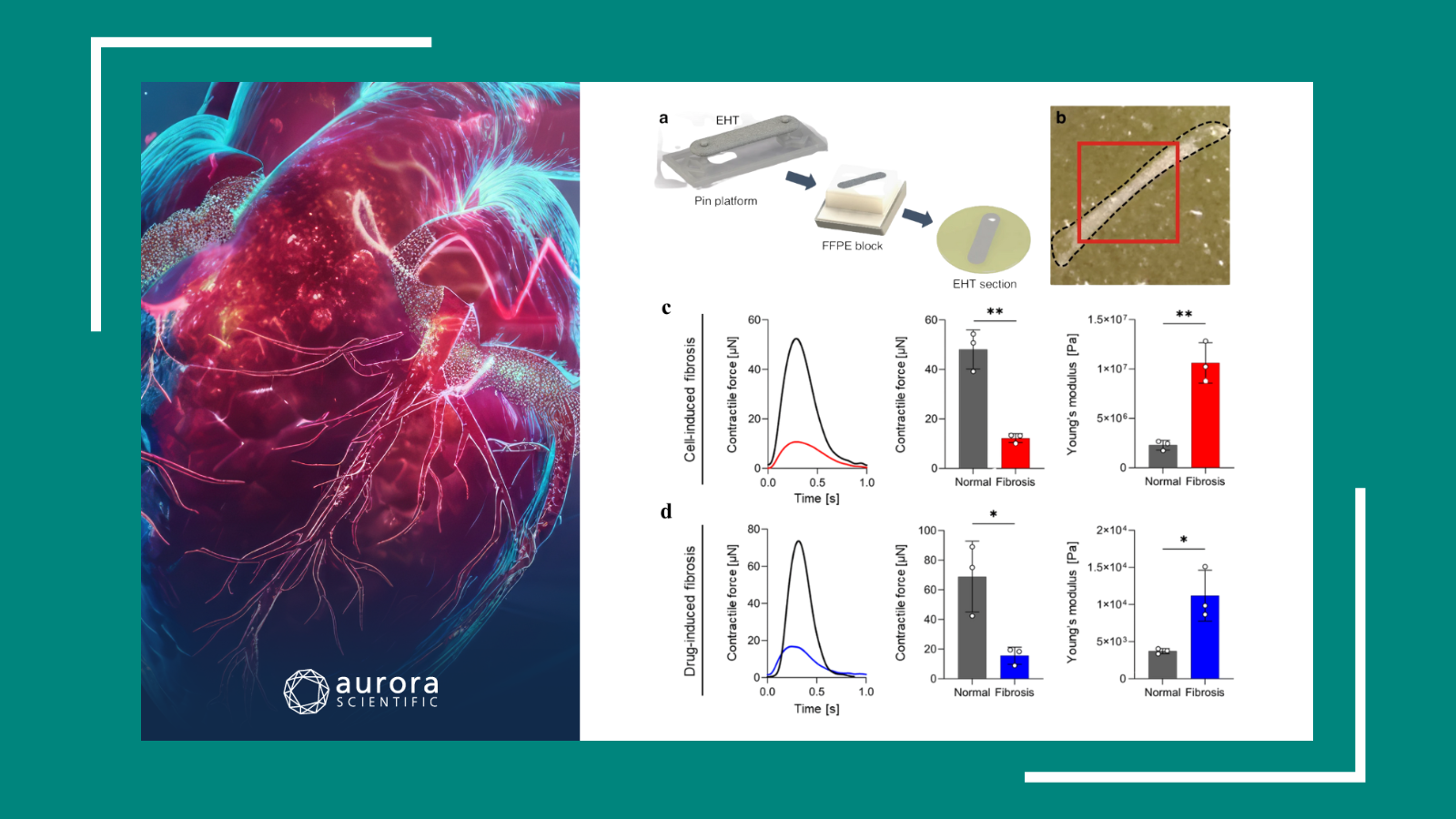
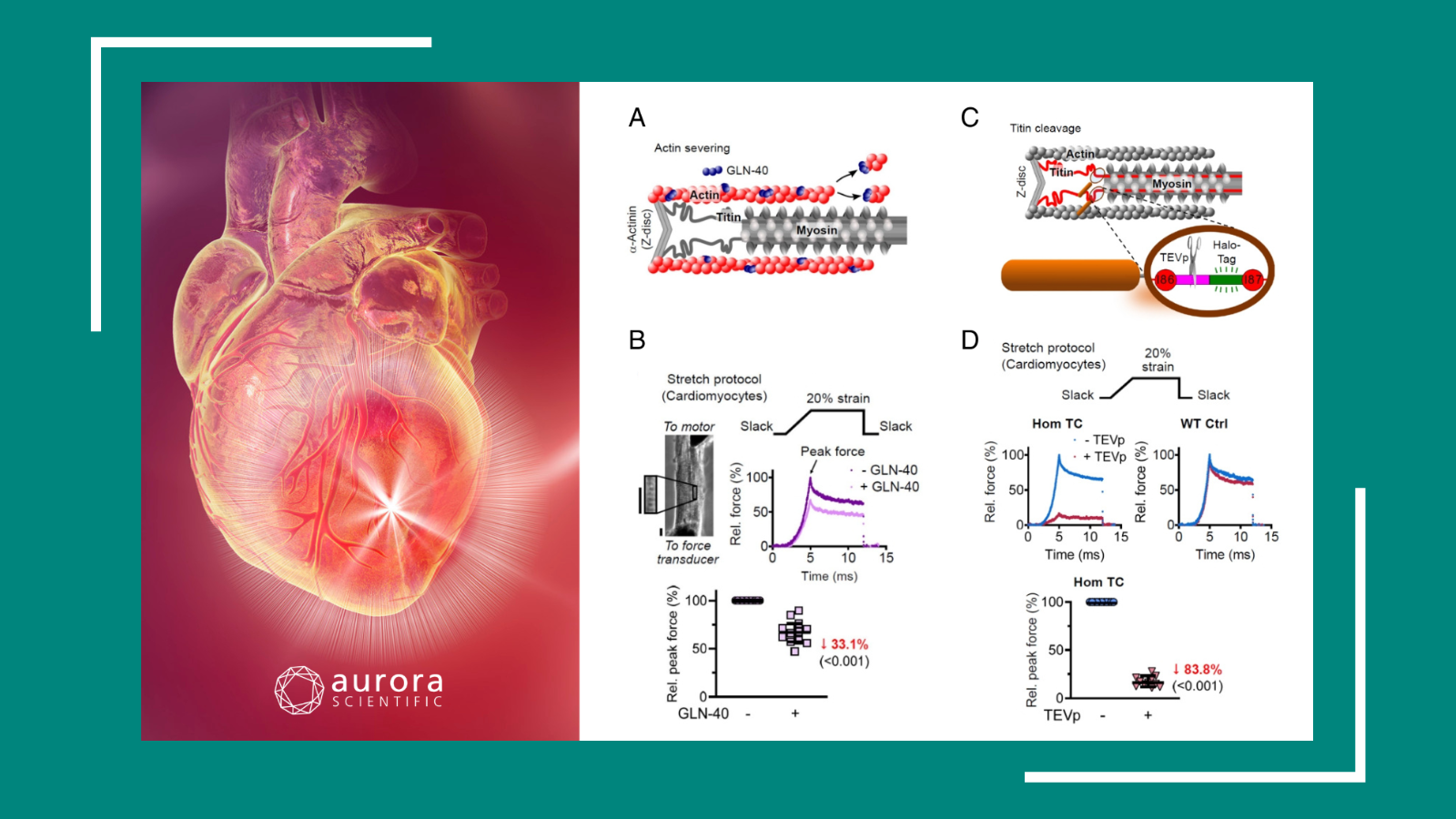
Heart-Hitting Discoveries
This publication review covers recent heart-hitting discoveries, including a novel method to assess heart tissue integrity, intricate relationships between heart function and redox balance, and the ...
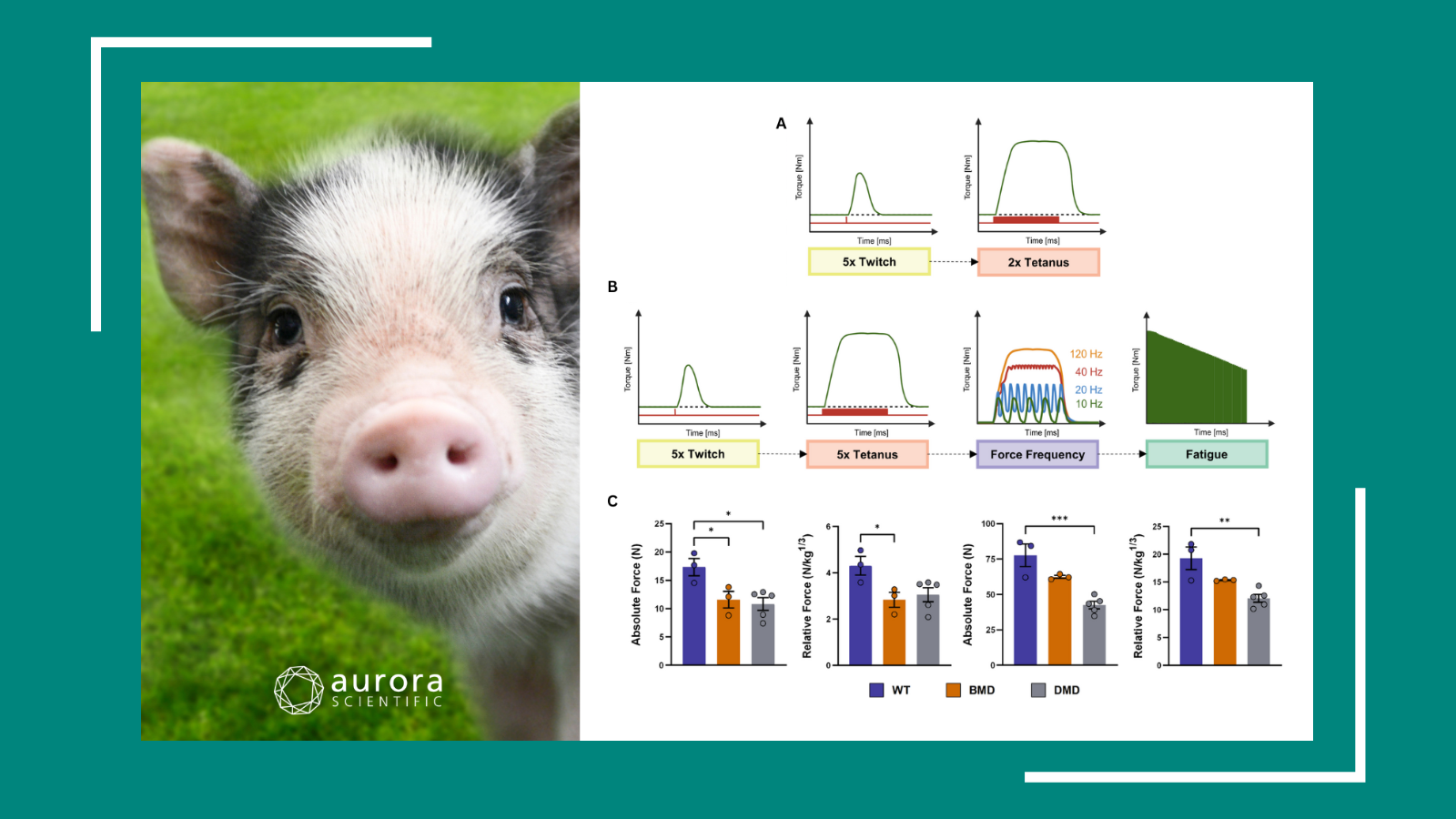
Pig-ture Perfect Progress
Kicking off 2026 with a lucky trot, this publication review highlights cutting-edge porcine research revealing how pigs help unravel the mechanics of muscle and heart function, from dystrophic rescue ...
2026 Winter/Spring Scientific Conferences and Meetings
The Aurora Scientific team is continuing to journey out and connect with researchers at scientific conferences and meetings all over the world this Winter and Spring! We are particularly thrilled to ...
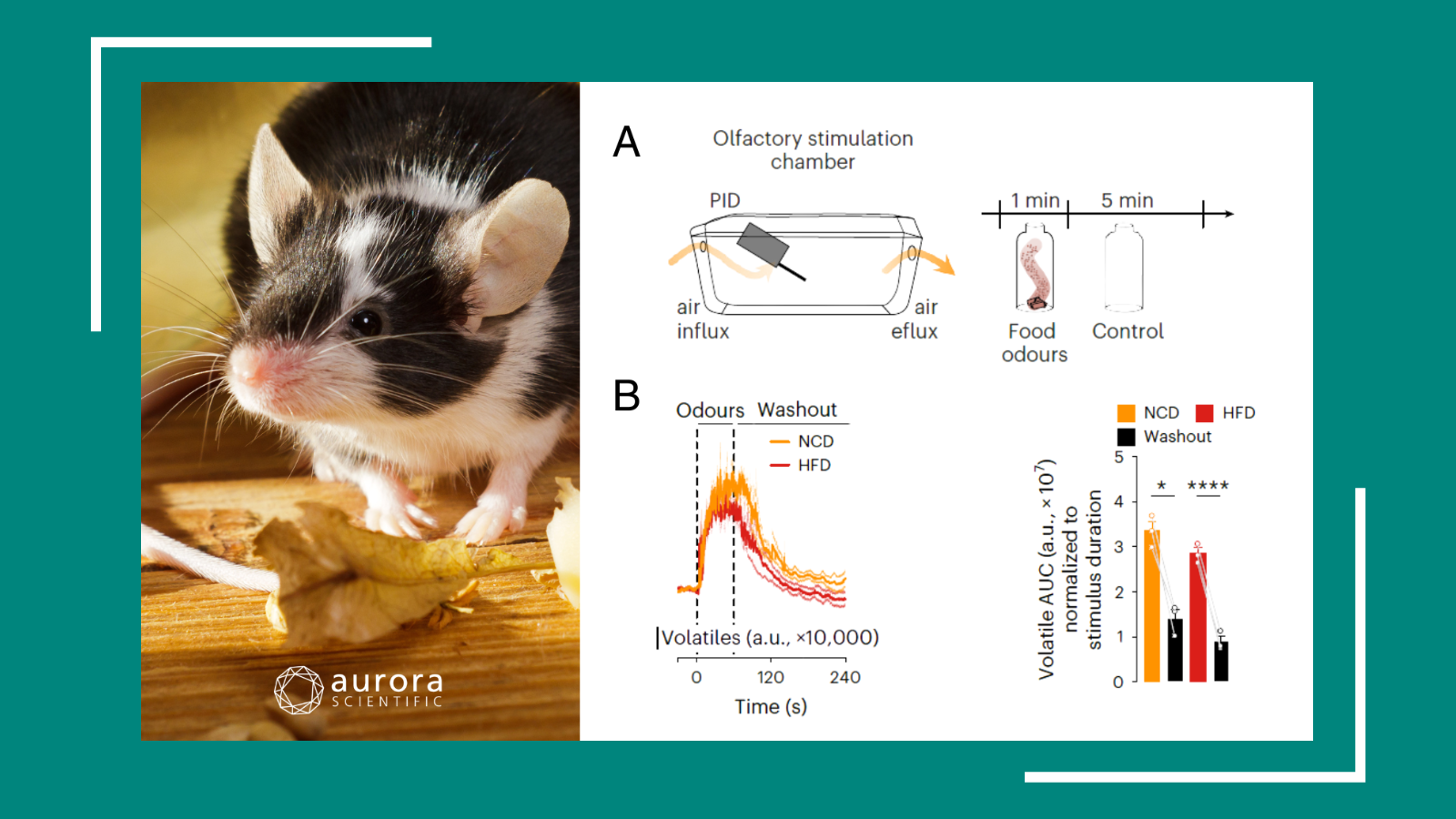
Best of 2025: Pushing Scientific Boundaries
Continuing our annual end-of-year tradition, this year’s final publication review spotlights the standout studies that captured the imagination of the field, pushing the boundaries of sensory ...
Calling in Reinforcements: Tube Repair of an ASI 400 Series Force Transducer
A step-by-step tech cast on how to perform a tube repair for Aurora Scientific's 400 Series Force Transducers, Katherine will share tips, tricks and best practices for best ...
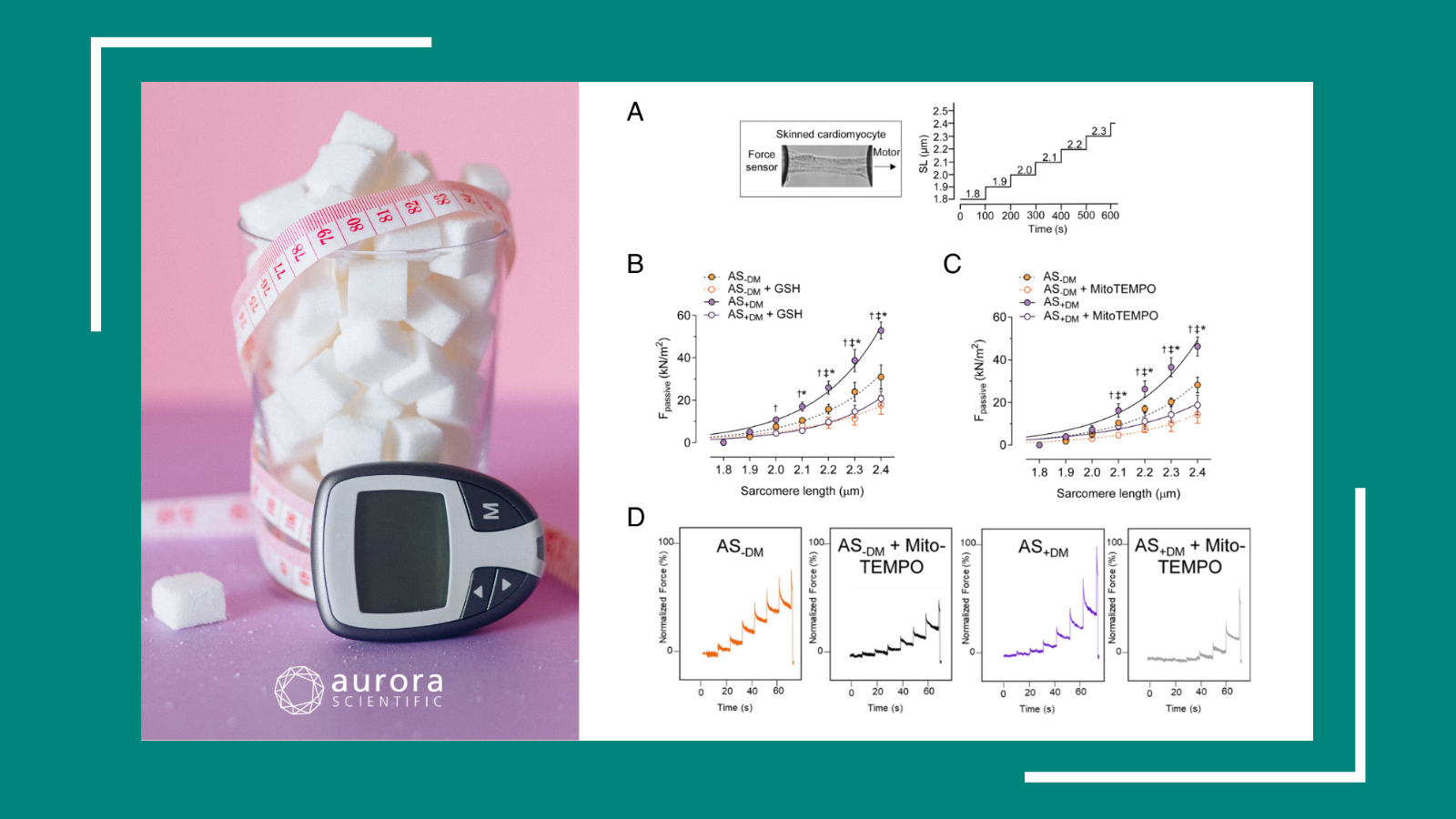
Diabetes Discoveries and Determinations
Over the years, diabetes has been the subject of growing global concern due to its effects on muscle, especially in the heart. In the following publication review, we delve into the latest ...
A Change of Heart: Novel Cardiac Findings
The Basic Cardiovascular Sciences meeting is held annually across the United States, offering a venue to explore, share, and collaborate on the latest cardiovascular insights. Without missing a beat, ...
2025 Winter/Spring Scientific Conferences and Meetings
The Aurora Scientific team is continuing to journey out and connect with researchers at scientific conferences and meetings all over the world this Winter and Spring! We are particularly thrilled to ...
Hearty Insights: Recent Advances in the Cardiac Field
Coming off the heels of this year’s Basic Cardiovascular Sciences Scientific Sessions (BCVS 2024), the following publication review focuses on an array of cardiac research, ranging from human ...
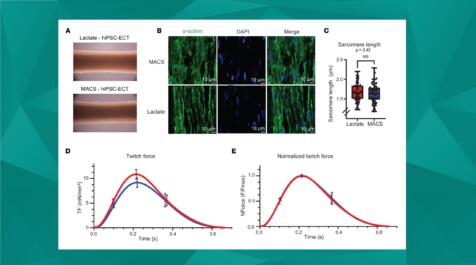
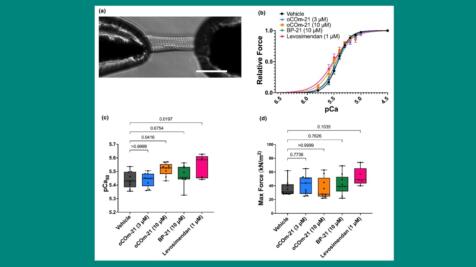
Spring into Action: Proteins of the Myofilament
In anticipation of the upcoming Myofilament Meeting, April’s publication review covers recent advances in the myofilament field. From the effects of inotropic agents on cardiac myofilament Ca2+ ...
Moving Mountains: Recent Feats in Muscle Physiology
As we March towards the 2024 American Physiology Summit, this month’s publication review covers recent advancements in the realm of muscle physiology, including the development of an improved ...
Tackling the Heart of the Issue: Advances in Cardiovascular Research
February notably marks “Heart Month”, aiming to highlight the importance of cardiovascular health and its critical implications on our overall wellbeing. Tackling the heart of the issue, several ...
2024 Spring/Summer Scientific Conferences and Meetings
The Aurora Scientific team is continuing to journey out and connect with researchers at scientific conferences and meetings all over the world this spring and summer! We are particularly thrilled to ...
Unlocking Heart Health: Revolutionizing Diastolic Function through Integrative Muscle Physiology at Wayne State University
Dr. Charles Chung is an Associate Professor of Physiology at Wayne State University. Using integrated physiology, analyzing data from the molecular level to the whole muscle, his laboratory aims to ...