Image courtesy of Siri et al. (2019).
Disorders like gastroparesis, gastroesophageal reflux disease (GERD), and inflammatory bowel syndrome (IBS) are very common causes of illness in developed countries. Digestive organ distension and stretching can be a source of pain in these disorders. Additionally, these conditions are often characterized by changes in the contraction of smooth muscle tissue within various digestive organs, leading to dysregulated gastrointestinal motility. More research is needed to analyze the link between muscle stretching, tension, and compression, and the mechanical function of the organs as a whole. This publication review highlights two studies that advance our understanding of the biomechanical properties of muscle tissue in the stomach and in the distal colon and rectum (colorectum).
On a Coupled Electro-Chemomechanical Model of Gastric Smooth Muscle Contraction
Klemm et al. (2020) created a three-dimensional model of smooth muscle contraction in the stomach. The authors incorporated information about regulation of smooth muscle cells (SMCs) by interstitial cells of Cajal (ICC), changes in calcium concentrations within SMCs, and force measurements. The resulting model provided information about the mechanical and electrochemical processes that drive gastric motility. In order to measure the mechanical properties of the mucosal and muscular layers of the stomach wall, the authors isolated smooth muscle strips from the stomach of pigs. Using our 805A in-vitro muscle apparatus and 305C dual-mode muscle lever, the researchers measured the active and passive stretch-stress responses of the tissue strips. The authors found that this mechanical activity in the stomach helps regulate the ICC and SMC membrane potential, which in turn influences intracellular calcium levels. Altogether, the model helps describe the response of the stomach muscle to move food.
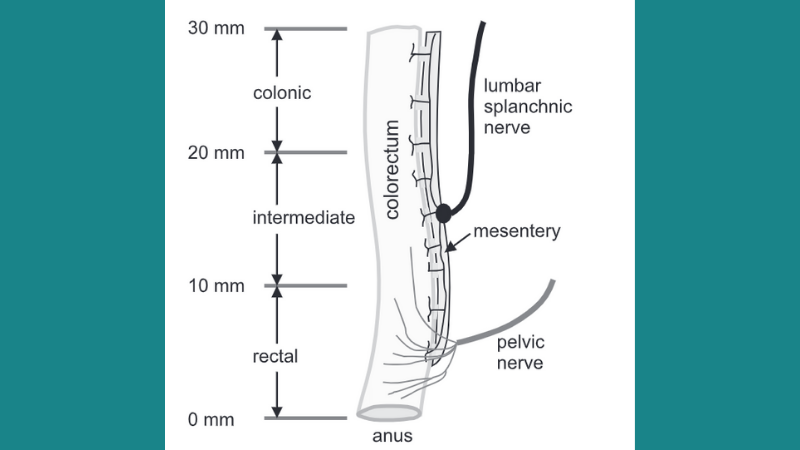
Differential Biomechanical Properties of Mouse Distal Colon and Rectum Innervated by the Splanchnic and Pelvic Afferents
In this article, Siri et al. (2019) analyze how muscle mechanics in different regions along the length of the colorectum may influence neural encoding and pain perception. Two sets of afferent neurons play an important role in colorectal mechanotransduction, or transmitting mechanical stimuli from the colorectum to the central nervous system. The distal colon is primarily innervated by the lumbar splanchnic nerves (LSN), while the rectum is innervated by the pelvic nerves (PN). These sets of nerves can sense mechanical stretching of the innervated muscle as well as smooth muscle contractions. The authors isolated tissue strips from the colon, rectum, and intermediate tissue of mice. Using our 300D dual-mode muscle lever, the authors performed biaxial mechanical stretch tests to better characterize their biomechanical properties. They also used second harmonic generation (SHG) imaging tests to measure the orientation of collagen fibers in different layers of the colorectal wall. The researchers reported differential stretch-stress responses within the different colorectal regions. They also found that the colorectum is nearly twice as stiff in the axial direction compared to the circumferential direction, which are consistent with their findings that collagen fibers in the submucosa are aligned axially. This report suggests that local tissue biomechanics in different parts of the colorectum help influence different neural encoding.