When the supply of oxygen to tissue is restricted or stopped, ischemia/reperfusion (IR) injury can cause extensive damage to muscle tissue. Although much research has been done to better understand recovery following IR injury, the underlying mechanisms of IR-induced neuromuscular damage are still poorly understood.
Surgical rodent models that induce ischemia in the hind limb are commonly used, and within this strategy many variations exist. The two studies below take a divergent approach to the topic: the first looks into the early skeletal muscle injury response, while the other uses a longitudinal approach to characterize the role of mitochondrial oxidative stress in a model of tourniquet-induced IR.
Strain-Dependent Variation in Acute Ischemic Muscle Injury
Historically, ischemia research has largely focused on the recovery period following injury – the days to weeks following ischemia. As a result, the severity has been mostly attributed to the degree of perfusion reduction and to the ability of the tissue to regenerate. However, recent research suggests that, even with a similar reduction in perfusion and oxygen saturation, the severity of ischemic injury at 7 days can vary between mice strains.
To investigate whether this difference can be attributed to strain-dependent sensitivity to ischemic injury, Schmidt et. al. looked at the early ischemic injury response in two mouse strains known to differ greatly in their postischemic recovery: BALB/cJ (B/c) and C57BL/6J mice.
To do this, the authors induced acute hind limb ischemia and measured early differences in perfusion, oxygen saturation, muscle morphology, dystrophin immunostaining and muscle function for the two strains. 6 hours following ischemic injury, they found that perfusion was comparable between B/c and C57 mice, but B/c mice exhibited a greater loss of dystrophin-positive immunostaining and more severe muscle tissue necrosis.
To assess muscle function, they mounted single extensor digitorum longus and soleus muscles on the Aurora 300B-LR Dual-Mode lever system 6 hours after ischemia. Isometric tension was assessed for each muscle, however for both the B/c and C57 strain, they observed complete functional impairment for the muscles from both strains.
The authors write that the severity of early skeletal muscle in B/c mice:
“cannot be explained by the degree of perfusion reduction alone.”
They conclude that the B/c strain may have an inherent sensitivity to ischemic insult, suggesting that genetics may be a critical determinant of tissue sensitivity to ischemic injury.
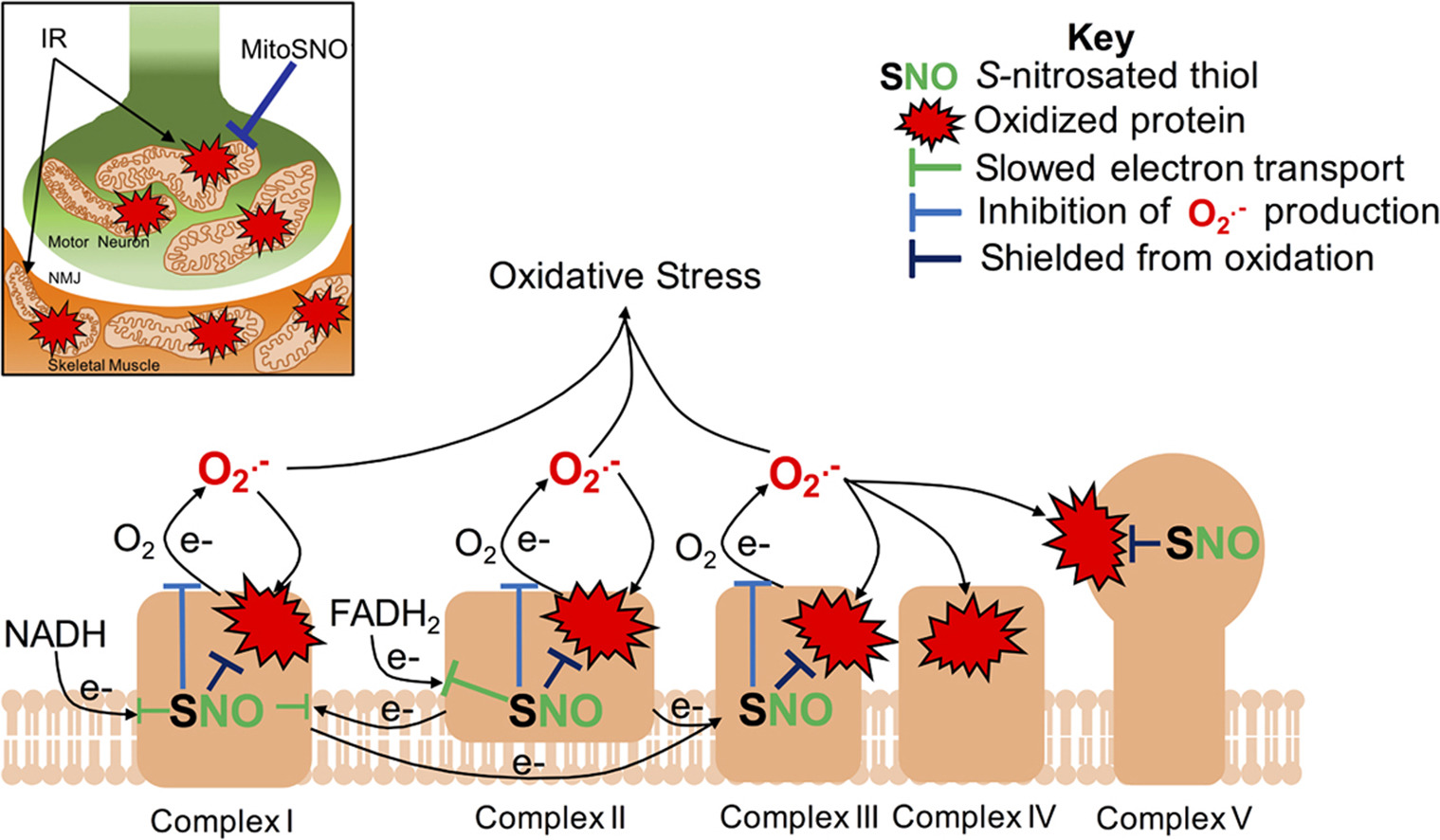
Mitochondrial protein S-nitrosation protects against ischemia reperfusion-induced denervation at neuromuscular junction in skeletal muscle
The mechanisms underlying ischemia-reperfusion-induced neuromuscular damage are still unclear. However, it is known that oxidative stress plays a pivotal role in ischemia-reperfusion injury. Recent research suggests that enhancement of mitochondrial protein S-nitrosation, or SNO, inhibits mitochondrial respiration and has a cytoprotective effect in the context of myocardial infarction.
In this study, Wilson et. al. sought to investigate whether mitochondrial SNO could attenuate the severity of neuromuscular damage in a tourniquet-induced model of ischemia-reperfusion. For this model, a tourniquet was applied over the femur of a mouse for 1 h – a duration comparable to clinical guidelines which use a tourniquet to control blood flow in humans.
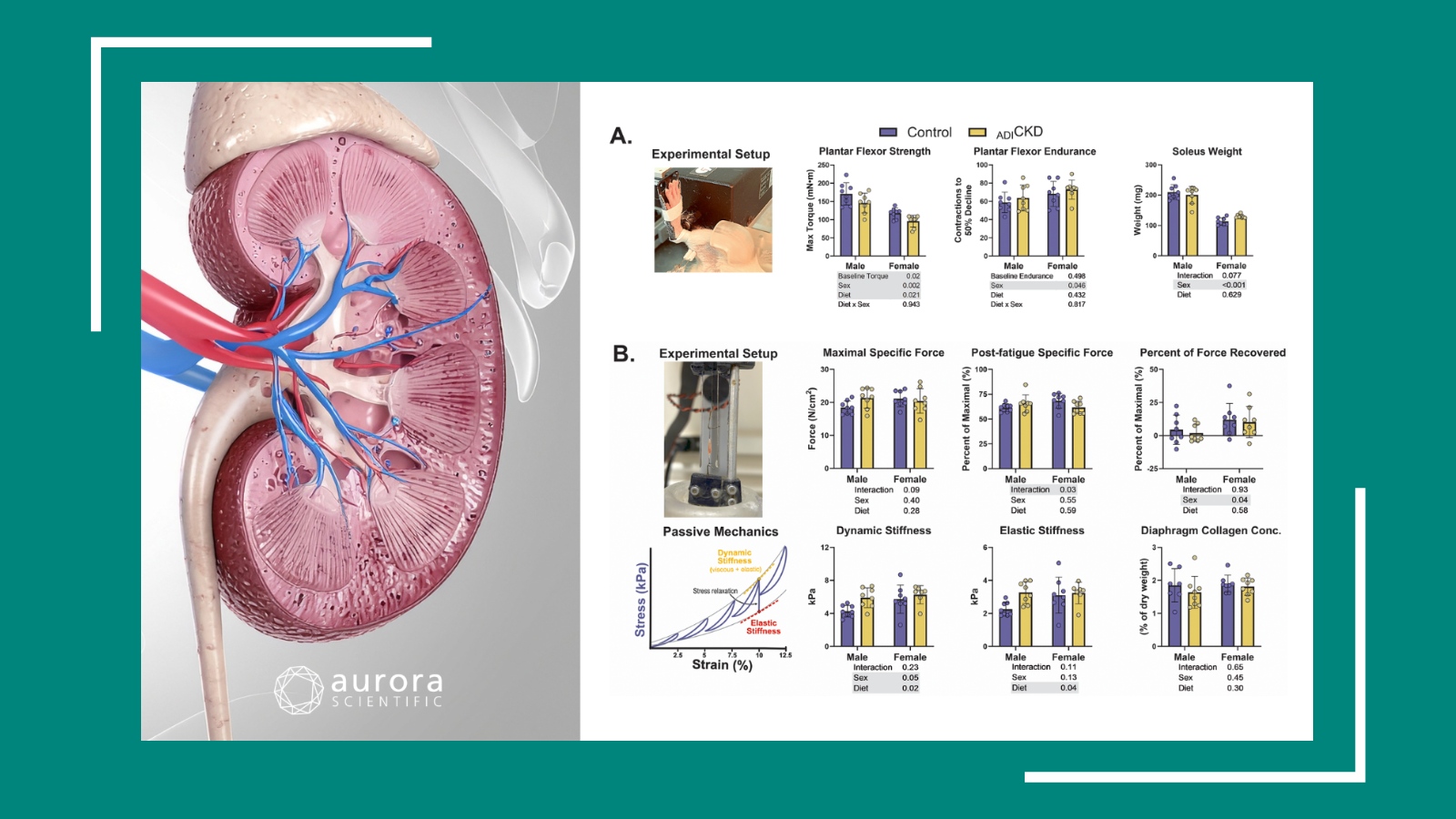
In a group of mice, hind limbs were injected with a mitochondria-targeted S-nitrosation enhancing agent (MitoSNO). Then, for 28 days following ischemic injury, the authors performed a longitudinal footplate study, measuring isometric torque of the mice’s plantarflexors in-vivo using the 1300A Whole Animal System. They found that mice that received the MitoSNO injection experienced a reduction in neuromuscular damage, lessened denervation at the neuromuscular junction and recovered their strength more quickly than mice that did not.
Considering the neuroprotective effect mitochondrial protein S-nitrosation has in the context of myocardial infarction and now, ischemia/reperfusion injury, MitoSNO represents an exciting avenue for treatment in the future.