As our collective understanding of biomaterials and stem cells has improved, cardiac tissue engineering has emerged as a promising potential treatment for heart disease and powerful tool for in vitro research. The basic premise is that, given the right conditions, stem cells will differentiate into healthy, mechanically functional heart tissue. This heart tissue can then be transplanted onto an infarcted heart, restoring function and preventing further remodelling and recurrence.
However, these conditions are a challenge to achieve. Research is currently being done to develop substrate and scaffold formulations which accurately mimic the heart’s natural properties. Two recent articles provide a fascinating window into cardiac tissue engineering, illustrating the development of natural and synthetic scaffolds that work and the analysis to support it.
Head-to-head comparison of two engineered cardiac grafts for myocardial repair: From scaffold characterization to pre-clinical testing
Perea-Gil et al. published an article in Nature Scientific Reports comparing two cardiac grafts using decellularized myocardial and pericardial tissue samples. To generate cardiac scaffolds, the team decellularized and sterilized cardiac tissue samples. These scaffolds were then repopulated using porcine adipose tissue mesenchymal stem cells (pATMSCs).
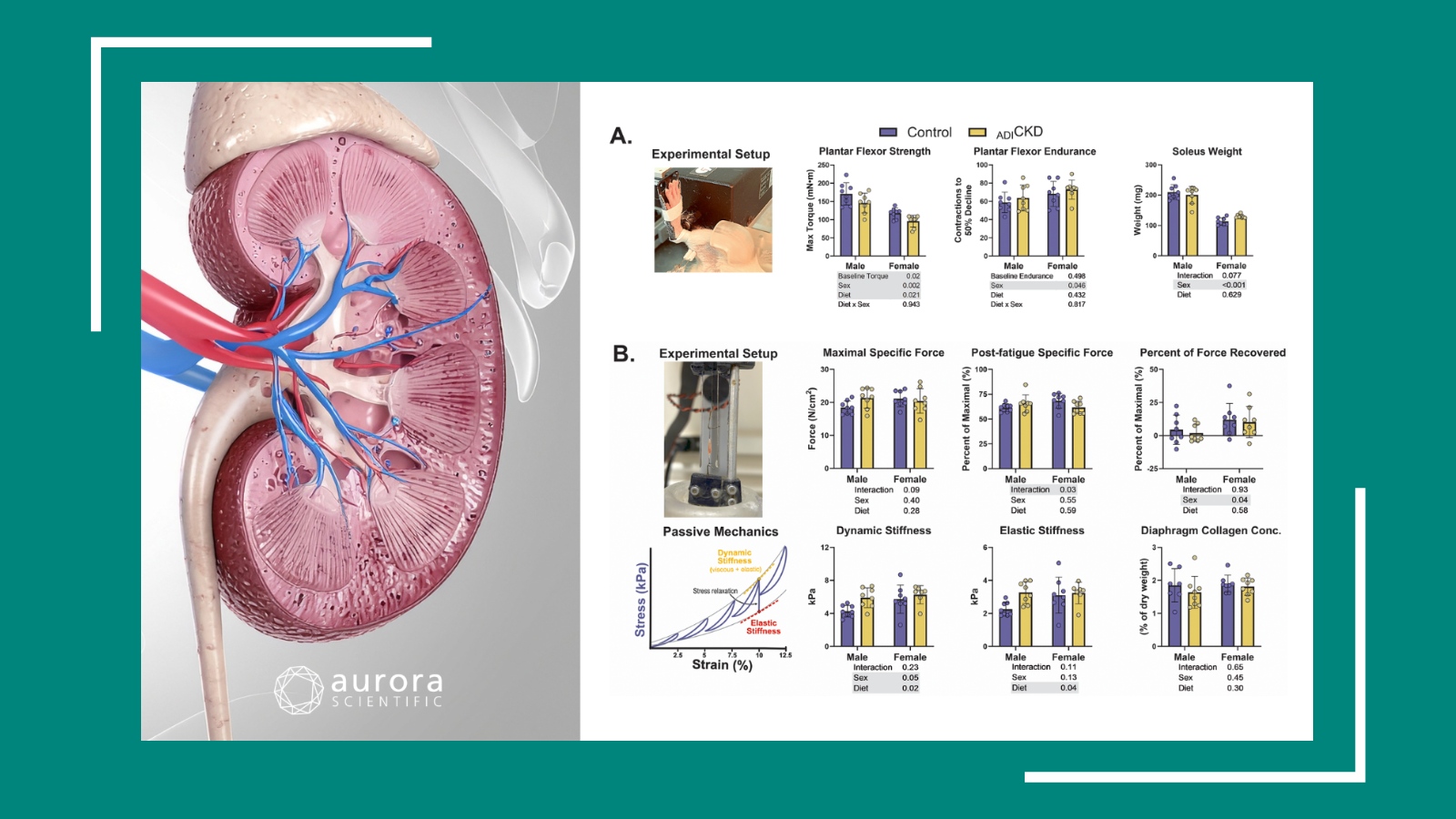
To assess the mechanical and tensile properties of the heart, the team cut strips of myocardial and pericardial tissue and used the Aurora Scientific 300C-LR to measure the length, applied force and by extension stiffness. They found that,
“The structure, macromechanical and micromechanical scaffold properties were preserved… except for recellularized myocardium micromechanics that were ∼2-fold stiffer than native tissue and decellularized scaffolds.”
In addition to in vitro testing, they evaluated the pericardial and myocardial grafts in a porcine MI swine model for 40 days. The therapy was a clear success – they report,
“the engineered grafts integrated with the underlying myocardium, with signs of neoinnervation and neovascularization, and improved cardiac function post-MI.”
Optimizing Blended Collagen-Fibrin Hydrogels for Cardiac Tissue Engineering with Human iPSC-derived Cardiomyocytes
While Perea-Gil et al. used scaffolds made from decellularized tissue samples, Kaiser et al. discuss the development and characterization of a collagen and fibrin hydrogel in an article published in ACS Biomaterials Science and Engineering. The team sought to explore the impact of different scaffold formulations on compaction, stiffness and force production. The authors note that while collagen hydrogels and fibrin hydrogels have frequently been used for cardiac tissue engineering, there is no evidence that a blend using both has been evaluated.
More importantly, while most studies have been relatively limited in scope, manipulating and evaluating the effect of a single variable, Perea-Gil et al. looked at several: collagen concentration, fibrin concentration, seeding density and cardiomyocyte purity, each at a low, medium and high level.
The team prepared blended collagen and fibrin hydrogels, seeded them with human induced pluripotent stem cell-derived cardiomyocytes (hiPSCs) and measured the constructs’ mechanical properties (particularly stiffness, compaction and force production) using the 1500A Isolated Muscle System from Aurora Scientific.
Using their data, they generated a predictive model characterizing the complex relationships between scaffold composition, seeding density and cardiomyocyte purity. They summarize,
“It is our aim that this study will serve as a foundation for the development of more sophisticated and highly functional engineered cardiac tissues in the future.”
There is no single ‘recipe’ for a perfect scaffold – whether for preclinical research or medical treatment, the ideal scaffold will depend on the desired outcomes. Despite the progress being made in the research, many questions remain. But our understanding of cardiac tissue engineering is improving by leaps and bounds, and it’s only a matter of time before these questions have answers, both in the lab and in the clinic.